- Blog
- Printable pdf checkbook register template
- Samsung health sleep tracker
- Monk scripts achaea mudlet
- Skylum luminar 4
- Roadblock ipo
- Small tiny pinpoint red dots on skin dont ith
- 1player games
- Scott schwartz critical content
- Supraventricular tachycardia with ivcd
- Nch express invoice-
- Risk probability descriptors

All 6 patients showed myotonia at electromyography and pathological expansion of the nucleotide triplet CTG in locus 19q13.3 in the genetic study. In all cases, the first clinical suspicion of myotonic dystrophy arose in our centers, except for patients 5 and 6, who both had myotonia recognized several years before the onset of tachycardia. All had myotonia, distal muscular weakness, and hyporeflexia, and except for patient 2, all had cataracts. They had no other history of interest, and none of them presented cardiac symptoms, apart from those related to tachycardia episodes.Īll patients showed the characteristic phenotype of frontal baldness and distal and parietal muscle atrophia. Two patients had a family history of sudden death. Their main clinical characteristics are displayed in the Table. Six consecutive patients with myotonic dystrophy were referred to our centers for evaluation and treatment of sustained wide QRS complex tachycardia. To this end, we tested the relationship of this mechanism with clinical monomorphic sustained ventricular tachycardias in 6 consecutive patients with myotonic dystrophy, 5 of whom had no apparent valvular or myocardial dysfunction. We postulated that cardiac involvement in myotonic dystrophy is an ideal substrate for bundle-branch reentry. 10 11 In addition, no standard therapy for these arrhythmias has been established. 1 2 5 6 However, the mechanism of ventricular arrhythmias in this setting has not been determined, and reentry related to areas of damaged myocardium is thought to be the most plausible explanation. This observation, together with reports of spontaneous ventricular tachycardia, 5 6 7 8 9 raises the possibility that ventricular arrhythmias play a major role in the mortality of these patients. Although commonly attributed to conduction block, sudden death has been seen in patients with pacemakers. 1 2 3 4 There is also a high incidence of sudden death, which makes it a significant unsolved clinical problem. 1 Cardiac involvement is frequent and is manifested as a selective and extensive impairment of the conducting system, which typically is not associated with apparent structural heart disease. Myotonic dystrophy is the commonest muscular dystrophy occurring in adult life, with a prevalence of 1 in 8000. This is especially true if no apparent heart disease is found.
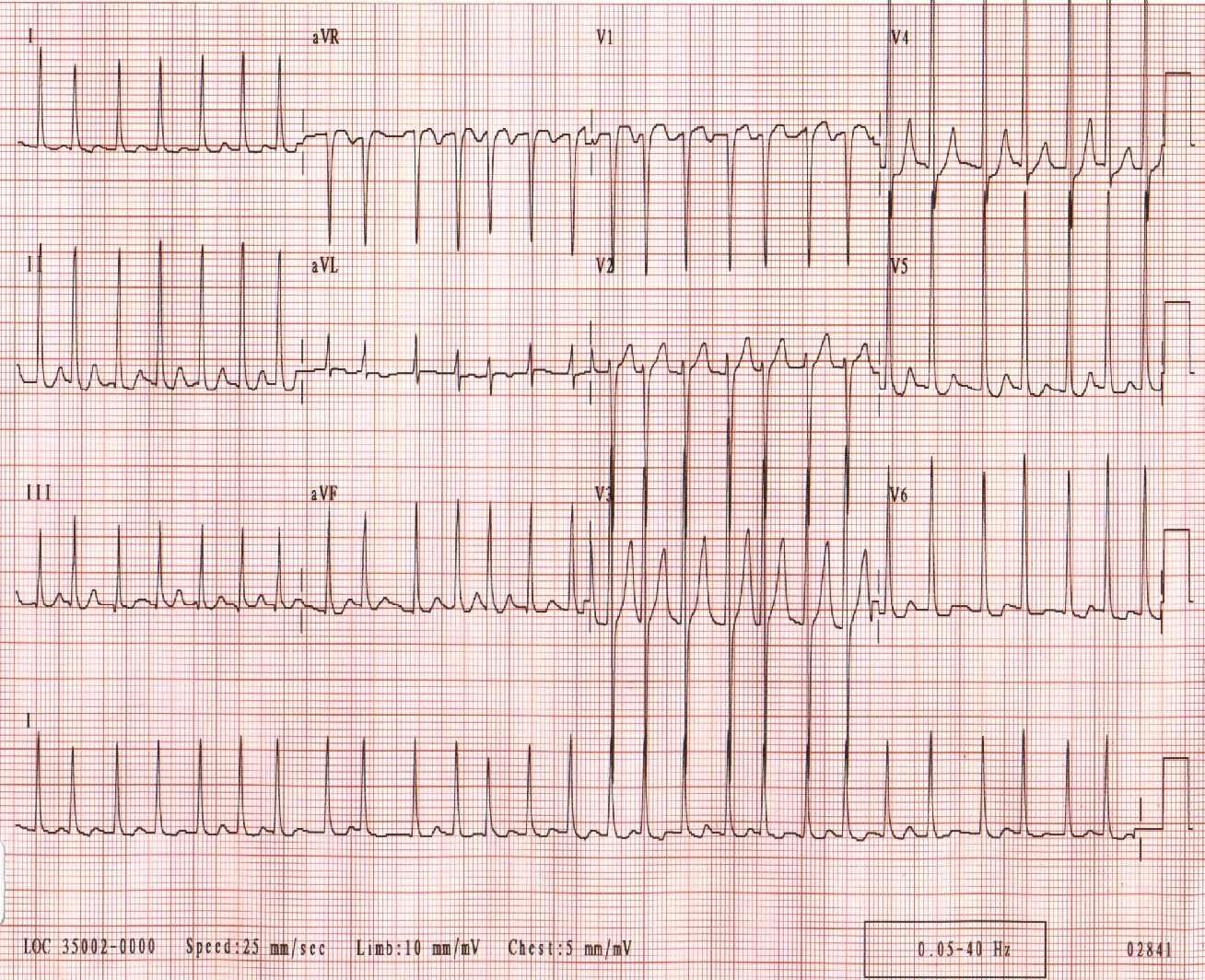
Because catheter ablation will easily and effectively abolish bundle-branch reentrant tachycardia, myotonic dystrophy should always be considered in patients with sustained ventricular tachycardia. Ventricular tachycardia was no longer inducible after bundle-branch ablation, except for a nonclinically documented and nonsustained ventricular tachycardia in the only patient who had apparent structural heart disease.Ĭonclusions-A high clinical suspicion of bundle-branch reentrant tachycardia is justified in patients with myotonic dystrophy who exhibit wide QRS complex tachycardia or tachycardia-related symptoms. In 1 patient, 2 other morphologies of sustained tachycardia were also inducible, neither of which had ever been clinically documented, and both had a bundle-branch reentrant mechanism. Clinical tachycardia was inducible in all patients and had a bundle-branch reentrant mechanism.


Particular attention was paid to establish whether bundle-branch reentry was the tachycardia mechanism, and when such was the case, radiofrequency catheter ablation of either the right or left bundle branch was performed. Methods and Results-We studied 6 consecutive patients with myotonic dystrophy and sustained ventricular tachycardia by means of cardiac electrophysiological testing. However, their precise mechanism is unknown, and their definitive therapy remains to be established. Customer Service and Ordering Informationīackground-Ventricular arrhythmias have been documented and linked to the high incidence of sudden death seen in patients with myotonic dystrophy.Stroke: Vascular and Interventional Neurology.Journal of the American Heart Association (JAHA).Circ: Cardiovascular Quality & Outcomes.Arteriosclerosis, Thrombosis, and Vascular Biology (ATVB).
- Blog
- Printable pdf checkbook register template
- Samsung health sleep tracker
- Monk scripts achaea mudlet
- Skylum luminar 4
- Roadblock ipo
- Small tiny pinpoint red dots on skin dont ith
- 1player games
- Scott schwartz critical content
- Supraventricular tachycardia with ivcd
- Nch express invoice-
- Risk probability descriptors
